An Award-Winning Culture of High-Quality Care
Awards and Recognition
Monument Health is nationally-recognized by trusted health care industry organizations like CMS Star Ratings, Leapfrog, U.S. News and World Report and American Heart Association.
Building a Culture of Continuous Improvement
At Monument Health, quality is more than a standard—it’s a promise. Every person in our organization plays a role in delivering high-quality care. Our quality teams, clinicians, support staff and every person who touches a patient’s experience are the reason we deliver excellence, every day.
A Team United for Quality
It’s about all of us, working together to ensure safer systems, better outcomes and meaningful human connection. That means the often invisible, though always impactful work that happens behind the scenes: reviewing and sharing data, refining policies and protocols, leading new quality and safety initiatives. It means constantly asking, “How can we do better?”


Monument Health Initiatives
Infection Prevention
Monument Health implemented best practices insertion procedures and maintenance in dressing change procedures, which resulted in fewer Central Line Associated Blood Stream Infections (CLABSI) and Clostridium difficile (C. diff). Antimicrobial Stewardship, environmental cleaning processes and use of ultraviolet lights resulted in an additional decrease in C. diff infections.
Result: National recognition from the Agency for Healthcare Research and Quality (AHRQ) for its decreases in CLABSI and Catheter Associated Urinary Tract Infections (CAUTI).
Hand Hygiene

Sanitize Now and Protect (SNAP)
The Centers for Disease Control and Prevention (CDC) says washing hands is one of the most effective ways to prevent the spread of diseases and infections.
Our health care workers are required to wash or sanitize their hands before and after caring for each patient. More than 130,000 hand hygiene observations are monitored each month to help our efforts to reach 100 percent hand hygiene compliance.
Patients and visitors should wash their hands before eating, after using the restroom and after touching any surface in the hospital room.
Stroke Care
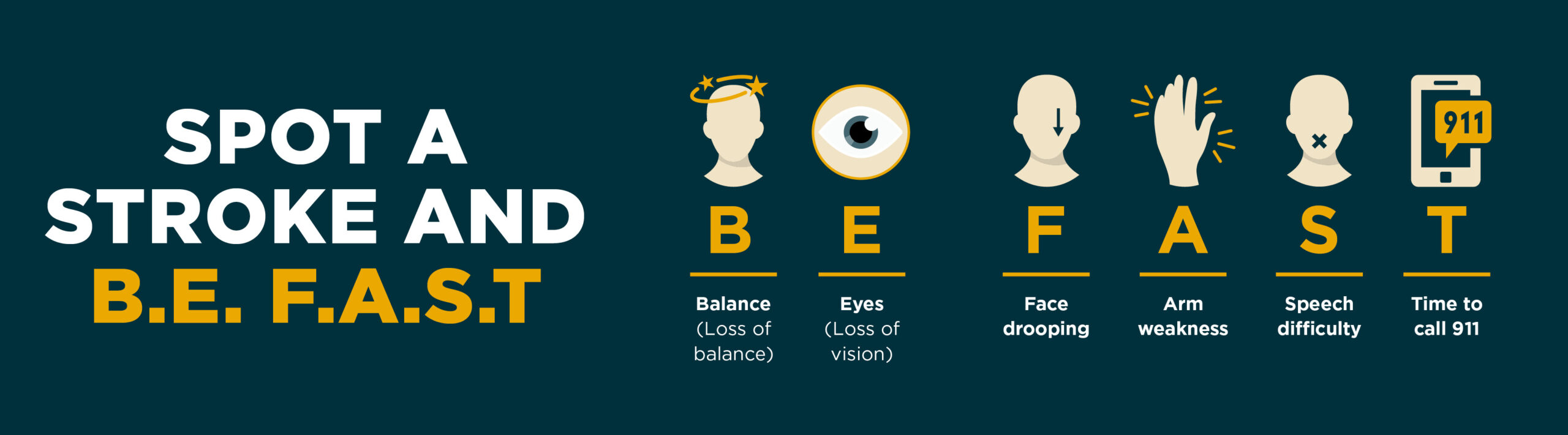
Monument Health follows Joint Commission and American Heart Association guidelines to provide efficient and quality care to patients experiencing a stroke. Utilizing a multidisciplinary response team allows the patient to receive stroke interventions based off of personal medical history and current symptoms which provides better outcomes for the patient.
The recommended time is within one hour.
Result: 55-minute average response time.
Diabetes Education
Diabetes affects a large number of western South Dakota residents. To help fight diabetes, we have established regional outreach clinics throughout western South Dakota; standardized case management for care and testing; introduced Diabetes Champions to help patients with assessment, care and education and leveraged community and national resources to assist patients get medications.
Result: Levels of HbA1c, a key measure of blood sugar over time, have been improving in the region.
Leapfrog Hospital Safety Grade

Monument Health Rapid City Hospital earned a A Grade in the latest Leapfrog Group safety ratings. The Leapfrog Group, an independent nonprofit focused on patient safety, released its Fall 2025 Hospital Safety Grade, recognizing Rapid City Hospital with the highest safety grade of any South Dakota Hospital. The Hospital Safety Grade uses up to 30 performance measures to assign an “A, “B,” “C,” “D” or “F” to individual hospitals and updated twice per year.
ANCC Magnet Recognition for Nursing Excellence

Monument Health Rapid City Market attained Magnet designation from the American Nurses Credentialing Center (ANCC) in 2023. Magnet designation is the highest recognition for nursing excellence and quality patient care in the United States. This prestigious award, granted by the ANCC represents a commitment to quality and patient safety.
Magnet designation is an important recognition of quality patient care because it demonstrates the commitment to high standards of nursing practice and patient safety. This translates into better patient outcomes, such as lower infection rates, readmissions, and medical errors.






















